Cervical Cancer
What is Cancer?
The body is made up from millions of cells that are constantly dying and being replaced. Normally, cells divide in an orderly and controlled way. Cancer occurs when a cell divides and multiplies too rapidly. This produces a lump of abnormal cells known as a tumour. Tumours are either benign (non-cancerous) or malignant (cancerous). There are 200 different types of cancer and early detection can greatly increase the chances for successful treatment.
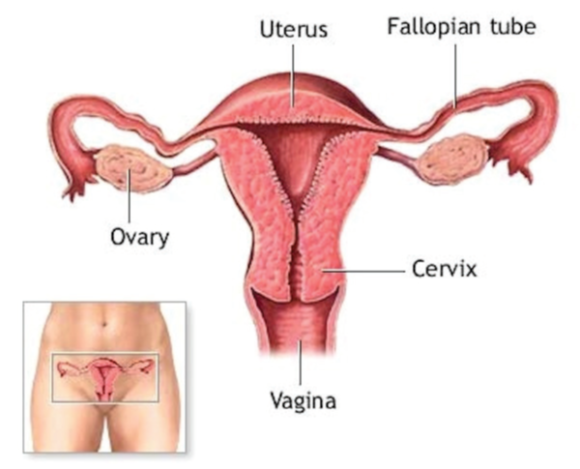
The cervix
The cervix is another name for the neck of the womb and it is covered by cells both on the inside and the outside of the womb. These cells can become cancerous leading to cervical cancer.
What causes cervical cancer?
Cervical cancer is often caused by the human papilloma virus (HPV). There are different types of HPV however not all types will cause cervical cancer. HPV is sexually transmitted and it is therefore very important to practice safe sex.
There are approximately 100 females a year in Northern Ireland diagnosed with cervical cancer and approximately 23 lives are lost each year to the disease.
Cervical Cancer
Symptoms of cervical cancer
Cancer of the cervix can take many years to develop, before it does, changes occur in the cells of the cervix. If you notice any of the following symptoms, please go immediately to your GP for further examination.
The most common symptom is abnormal bleeding outside of your period;
- Bleeding after sex
- Bleeding between periods
- Bleeding after the menopause (i.e. if your periods have stopped for 6 months or more)

Some women also have:
- A vaginal discharge that smells unpleasant
- Discomfort or pain in your lower pelvis
Precancerous cell changes do not usually have symptoms which is why it is so important to have a regular smear test.
Symptoms of Cervical Cancer
The HPV (human papilloma virus) vaccine
There are over 100 types of HPV but only 13 of these are known to cause cervical cancer and just two – types 16 and 18 – cause over 70% of the cases. The HPV vaccine is being offered to protect against types 16 and 18, which are the two most common types causing cervical cancer. To be fully effective the vaccination needs to be given before the start of sexual activity.
Who will receive the vaccine?
It is recommended the vaccination is given routinely as early as possible in schools to Year 9 girls aged 12 to 13. Having the vaccine reduces the risk of cervical cancer by 70%. The vaccination is given as three injections within six months to get the best protection, or within 12 months if an injection is missed. Like the vaccinations given to babies, it is important that the course is completed (all three doses) for it to work properly. The side effects are mild – mostly stinging or soreness where the injection is given in the arm, which soon wears off.
Cervical screening will still be essential to detect changes in the cervix caused by the other types of HPV and women will continue to be invited for screening as normal.
See more at: http://helpprotectyourself.info
The HPV (Human Papilloma Virus) Vaccine
The smear test
Women between the ages of 25 and 64 need to protect themselves from cervical cancer. You can do this by undergoing a simple cervical screening process called a smear test. The test shows if there are any cells in the cervix that are not normal.
All women who are registered with a GP are invited to attend for a smear test at least once every three or five years. The first invitation will be sent out just prior to a woman’s 25th birthday and every three years thereafter until 49. Women from the age of 50-64, will be invited once every five years.
It is very important to attend for your smear when called.

What is a smear test?
A smear test is a method of detecting abnormal cells on the cervix. Detecting and removing abnormal cervical cells can prevent cervical cancer.
The cervical screening test usually takes around five minutes to carry out. An instrument called a speculum will be gently inserted into your vagina to hold the walls of your vagina open so that your cervix is visible. A small soft brush will be used to take some cells from the surface of your cervix.
The sample of cervical cells will then be sent to a laboratory and examined under a microscope to see whether there are any abnormal cells. It’s very quick and most women feel only slight discomfort. The results of the test will be sent to you in the post and they aim to have the results back to you in 2 weeks.
The Smear Test
Risk factors for Cervical Cancer
HPV and Sex
The most important risk factor for cervical cancer is infection by the human papilloma virus (HPV).
Having sex at an early age and having several sexual partners can increase the risk of catching HPV and developing cervical cancer.
Smoking
Women who smoke double their risk of getting cervical cancer.
A weakened immune system
Women who are immunosuppressed (for example, those who are taking immunosuppressive drugs after an organ transplant or women who are HIV positive) may be at increased risk of developing cervical cancer.
Contraceptive pill
Long-term use of the contraceptive pill (for more than 5 years) can slightly increase the risk of developing cervical cancer.
Family history
If your mother or sister has had cervical cancer you are at greater risk that if no one in your family has had it.
Risk Factors for Cervical Cancer
Lower your risk of getting Cervical Cancer
- Regular cervical screening every 3-5 years is the best way to detect changes to the cells of the cervix
- The human papilloma virus (HPV) vaccination protects against the two strains of virus responsible for most cases of cervical cancer. The vaccine is given to girls when they’re 12 to 13 years old, with three doses given over a six-month period.
- Use a condom during sex as it can protect against HPV viruses linked with cervical cancer
- Give up smoking
Lower your risk of getting Cervical Cancer
Action Cancer provides…
Early Detection
Breast screening services and health checks available from the Big Bus and Action Cancer House in Belfast.
Support Services
Complementary therapy, acupuncture, counselling, life coaching, peer mentoring; and our Positive Living Programmes are available for those impacted by cancer in order to enhance quality of life and learn coping strategies.
Education
As a local charity with a focus on cancer awareness, prevention and detection the health promotion team deliver a range of services and programmes to schools, communities and workplaces across Northern Ireland.
